A root canal infection is an impairing oral condition that occurs when bacteria enter the inner chamber of the teeth due to trauma or untreated dental decay. The disease can develop quickly after the bacteria attack the fragile pulp substance of the internal layer of the tooth.
So, patients with a root canal infection should seek treatment at once. Root canal treatment is an effective procedure that cleans out the infected pulp and restores the tooth.
It can be difficult to differentiate a root canal infection from other dental problems. So, to be sure, explore the information below to understand root canal infections better.
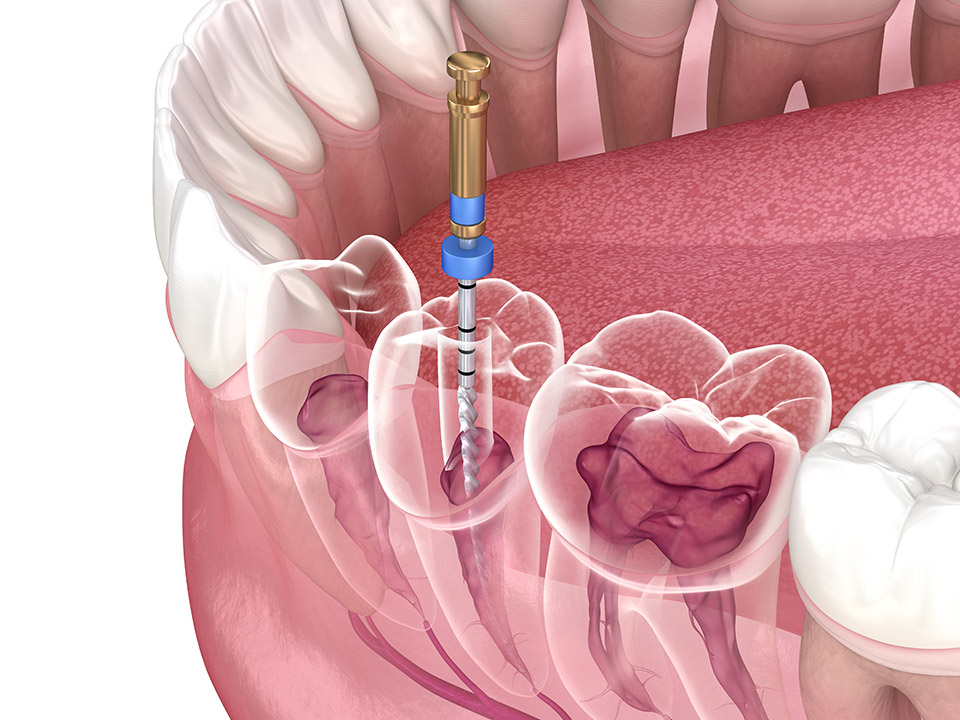
The Root Canal
The root canal is the inner part of the tooth between the tooth root and pulp, which contains blood vessels and nerves. The blood vessels carry nutrients to the nerves and teeth. The tooth’s nerves can sense different conditions such as heat, cold, and pressure.
Root canal therapy may need nerve excision as an essential part of the dental procedure in severe pulp infection and tooth decay.
It is not always simple to determine whether or not your tooth’s root canal is infected and requires therapy. Even people who do not need root canal therapy can display a wide range of symptoms. Only a skilled dentist can identify the less obvious signs of a root canal infection.
The Common Root Canal Infection Symptoms
Signs of a root canal infection include:
Acute Tooth Pain
Since the inner tooth material is so sensitive, infected root canals produce severe tooth pain. Occasionally, the root canal infection spreads and leads to a tooth abscess. When tooth pain becomes intolerable, you need immediate treatment.
However, not all tooth pain is related to the root canal. You do not need root canal therapy simply because you have severe tooth pain. Teeth that need root canal treatment may cause no pain at all.
In addition, dental disorders such as tooth fracture, tooth decay, sinus infection, periodontal disease, exposed dentin, and bruxism can also contribute to tooth pain. The key is to establish the exact site, onset, duration, and nature of the pain. Knowing whether the pain is subtle or strong and severe is crucial.
Identify whether the pain is acute and severe or dull and mild. The underlying issue, which causes some ache or discomfort, can last for weeks or even months. While most patients can pinpoint which tooth is hurting, the pain might occasionally be vague and generic. The following pain types are typical signs of a root canal infection:
- A pulsing toothache
- A lingering toothache
- Excruciating tooth pain when chewing something
- Pain that is so intense that it keeps you up at night
- A spontaneous pain that is either intermittent or continuous
- A pain that develops when you apply pressure to the infected tooth
- A pain that results from thermal stimuli, such as when you drink cold water right after drinking hot liquids, or vice versa
Gum Sensitivity and Swelling
These symptoms can present in different kinds and forms. The gum may appear normal with some tenderness, while at other times, a large mass is visible or palpable. In rare instances, the swelling might spread to the face or neck.
It frequently occurs with a toothache. However, the edema does not always signify infected root canals. And this makes deciding if root canal surgery is necessary challenging. The following are some swelling signs that could indicate root canal infections:
- Long-lasting swelling
- Pronounced swelling
- Recurrent pimples on the gums
- A tooth that feels a little taller than nearby teeth
- A boil that resembles a gum pimple on the gums in front of or on the root tip
Tooth Darkening
The development of a dark yellow, blue, or gray tone on a single darkened tooth may indicate a root canal infection. Fortunately, a discolored tooth is easy to spot.
Restricted blood supply causes the tooth to change color. Typically, tooth discoloration indicates pathogenic changes in the nerve region. So, a discolored tooth often points to a severely infected nerve.
As the infection progresses, the nerve becomes frailer and eventually dies. The dead nerve needs to be treated as soon as feasible. Otherwise, it will harbor bacteria that can cause various oral health issues.
Chronic Bad Breath and Dental Abscess
Bacteria can cause many foul-smelling illnesses, including root canal infections. Nasty bacteria can enter a root canal and multiply in the pulp chamber if the tooth enamel is weak from erosion, a cavity, or trauma. This will cause the pulp chamber to produce a foul smell. The pus, especially when draining and venting off, may also cause an unpleasant taste or odor in your mouth.
An infection in the gum can result in abscesses, which are pus-filled pockets. It begins as a little painful lump and grows with time. An abscess is challenging to treat. This is because your root canal infection is already widespread. So, it is critical to take prompt action if you notice a bulge beneath your gum.
Tips for Avoiding Root Canal Infections
There are various things you can do to lower the risk of a root canal infection:
- Rinse your mouth.
- Eat tooth-healthy foods.
- Avoid frequent snacking and sipping.
- Use dental floss and brush at least twice daily.
- Visit the dentist at least twice annually to maintain your teeth’ general health and identify any early signs of illness or decay.
- Ask about antibacterial treatments, especially if you have a vulnerable tooth or teeth.
- If you observe any early indications of infection, contact your dentist immediately.
To Sum It Up
Our bodies are very effective at fighting illnesses. However, the body is unable to produce antibodies for the tooth. If you exhibit any symptoms, you may require quick attention to prevent further problems, including tooth loss. Call our dental clinic and schedule an appointment with the dentist.
If the dead nerve is not treated quickly, the germs that cause infection will find a home there. The tooth’s nerves will likely die after the root canal becomes infected. To remove the dead pulp and treat the disease, the dentist might need to perform a root canal procedure and occasionally have to extract the dead tooth.